Acute infectious thyroiditis
| Acute infectious thyroiditis | |
|---|---|
| Other names: suppurative thyroiditis | |
Acute infectious thyroiditis (AIT) also known as suppurative thyroiditis, microbial inflammatory thyroiditis, pyrogenic thyroiditis and bacterial thyroiditis.[1][2][3]
The thyroid is normally very resistant to infection. Due to a relatively high amount of iodine in the tissue, as well as high vascularity and lymphatic drainage to the region, it is difficult for pathogens to infect the thyroid tissue. Despite all this, a persistent fistula from the piriform sinus may make the left lobe of the thyroid susceptible to infection and abscess formation.[1] AIT is most often caused by a bacterial infection but can also be caused by a fungal or parasitic infection, most commonly in an immunocompromised host.
Signs and symptoms
In most cases AIT is characterized by onset of pain, firmness, tenderness, redness or swelling in the anterior aspect of the neck.[4] Patients will also present with a sudden fever, difficulty swallowing and difficulty controlling the voice.[5] Symptoms may be present from 1 to 180 days, with most symptoms lasting an average of about 18 days. The main issue associated with the diagnosis of AIT is differentiating it from other more commonly seen forms of thyroid conditions.[4] Pain, fever and swelling are often much more severe and continue to get worse in people who have AIT compared to those with other thyroid conditions.[1]
Causes
Despite the thyroid gland being extremely resistant to infection, it is still susceptible to infection by various bacteria.[6] The cause can be almost any bacterium. Staphylococcus aureus, Streptococcus pyogenes, Staphylococcus epidermidis, and Streptococcus pneumoniae in descending order are the organisms most commonly isolated from acute thyroiditis cases in children. Other aerobic organisms are Klebsiella sp, Haemophilus influenza, Streptococcus viridans, Eikenella corrodens, Enterobacteriaceae,[4] and salmonella sp.[7] Occurrences of AIT are most common in patients with prior thyroid disease such as Hashimoto's thyroiditis or thyroid cancer. The most common cause of infection in children is a congenital abnormality such as pyriform sinus fistula.[5] In most cases, the infection originates in the piriform sinus and spreads to the thyroid via the fistula.[8] In many reported cases of AIT the infection occurs following an upper respiratory tract infection. One study found that of the reported cases of AIT, 66% occurred after an acute illness involving the upper respiratory tract.[6] Although the rates of infection are still very low, cases of AIT have been on the rise in recent years due to the higher occurrence of immune-compromised patients.[citation needed] Other causes of AIT are commonly due to contamination from an outside source and are included below.
Diagnosis
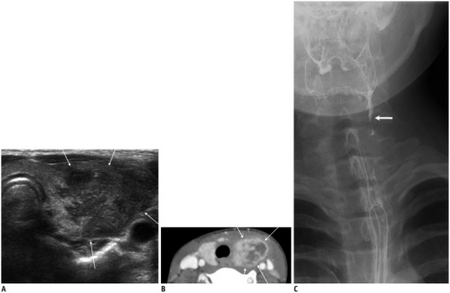
Patients who are suspected of having AIT often undergo tests to detect for elevated levels of white blood cells as well as an ultrasound to reveal unilobular swelling.[1][4] Depending on the age and immune status of the patient more invasive procedures may be performed such as fine needle aspiration of the neck mass to facilitate a diagnosis.[4] In cases where the infection is thought to be associated with a sinus fistula it is often necessary to confirm the presence of the fistula through surgery or laryngoscopic examination.[6] While invasive procedures can often tell definitively whether or not a fistula is present, new studies are working on the use of computed tomography as a useful method to visualize and detect the presence of a sinus fistula.[6]
Diagnostic tests
- Fever, redness, swelling
- Pain
- Blood tests of thyroid functions including TSH, T4 and T3 are usually normal [3]
- Ultrasonographic examination often shows the abscess or swelling in thyroid
- Gallium scan will be positive
- Barium swallow will show fistula connection to the piriform sinus and left lobe
- Elevated white blood cell count[3]
- Elevated erythrocyte sedimentation rate[3]
- Fine-needle aspiration
Subtypes of thyroiditis
| Subtypes | Causes |
|---|---|
| Hashimoto's thyroiditis, Chronic lymphocytic thyroiditis,[3] Chronic autoimmune thyroiditis, Lymphadenoid goiter[5] | Autoimmune[3] |
| Subacute lymphocytic thyroiditis, Postpartum thyroiditis, Sporadic painless thyroiditis,[3] Silent sporadic thyroiditis[5] | Autoimmune[3] |
| Acute infectious thyroiditis, Microbial inflammatory thyroiditis, Suppurative thyroiditis,[3] Pyrogenic thyroiditis, Bacterial thyroiditis[5] | Cause: Bacterial, Parasitic, Fungal[3] |
| de Quervain's thyroiditis, Subacute granulomatous thyroiditis,[3] Giant-cell thyroiditis, Pseudogranulomatous thyroiditis, Painful subacute thyroiditis,[5] | Viral[3] |
| Riedel's thyroiditis, Riedel's struma, Invasive fibrous thyroiditis | Unknown[3] |
Treatment
Treatment of AIT involves antibiotic treatment. Based on the offending organism found on microscopic examination of the stained fine needle aspirate, the appropriate antibiotic treatment is determined. In the case of a severe infection, systemic antibiotics are necessary.[2] Empirical broad spectrum antimicrobial treatment provides preliminary coverage for a variety of bacteria, including S. aureus and S. pyogenes. [4] Antimicrobial options include penicillinase-resistant penicillins (ex: cloxacillin, dicloxacillin) or a combination of a penicillin and a beta-lactamase inhibitor.[4] However, in patients with a penicillin allergy, clindamycin or a macrolide can be prescribed.[4] The majority of anaerobic organisms involved with AIT are susceptible to penicillin. Certain Gram-negative bacilli (ex: Prevotella, Fusobacteriota, and Porphyromonas) are exhibiting an increased resistance based on the production of beta-lactamase.[4] Patients who have undergone recent penicillin therapy have demonstrated an increase in beta-lactamase-producing (anaerobic and aerobic) bacteria. Clindamycin, or a combination of metronidazole and a macrolide, or a penicillin combined with a beta-lactamase inhibitor is recommended in these cases.[4] Fungal thyroiditis can be treated with amphotericin B and fluconazole.[2] Early treatment of AIT prevents further complications. However, if antibiotic treatment does not manage the infection, surgical drainage is required. Symptoms or indications requiring drainage include continued fever, high white blood cell count, and continuing signs of localized inflammation.[4] The draining procedure is also based on clinical examination or ultrasound/CT scan results that indicate an abscess or gas formation.[4] Another treatment of AIT involves surgically removing the fistula. This treatment is often the option recommended for children.[2] However, in cases of an antibiotic resistant infection or necrotic tissue, a lobectomy is recommended.[4] If diagnosis and/or treatment is delayed, the disease could prove fatal.[5]
Epidemiology
Acute infectious thyroiditis is very rare, with it only accounting for about 0.1–0.7% of all thyroiditis. Large hospitals tend to only see two cases of AIT annually.[2] For the few cases of AIT that are seen the statistics seem to show a pattern. AIT is found in children and young adults between the ages of 20 and 40. The occurrence of the disease in people between 20 and 40 is only about 8% with the other 92% being in children. Men and women are each just as likely to get the disease.[5] If left untreated, there is a 12% mortality rate.[2]
References
- ↑ 1.0 1.1 1.2 1.3 1.4 Melmed, Shlomo, Kenneth S. Polonsky, and P. R. Larsen. thyroiditis vs subacute thyroiditis diagnosis criteria[permanent dead link] "Acute InfectiousThyroiditis." Willams Textbook of Endocrinology. By Henry M. Kronenberg. 11th ed. Philadelphia: Elsevier, 2008. 945-47.
- ↑ 2.0 2.1 2.2 2.3 2.4 2.5 Lazarus, John, and James Hennessey. "Acute and Subacute, and Reidel's thyroiditis – Thyroid Disease Manager". Archived from the original on 2012-04-29. Retrieved 2012-04-20. "Acute and Subacute, and Reidel’s Thyroiditis." Ed. Leslie J. De Groot. The Thyroid And Its Diseases. 6th ed. New York: Elsevier, 1996.
- ↑ 3.00 3.01 3.02 3.03 3.04 3.05 3.06 3.07 3.08 3.09 3.10 3.11 3.12 Slatosky, D.O., J; Shipton, B; Wahba, H (Feb 15, 2000). "Thyroiditis: differential diagnosis and management". American Family Physician. 61 (4): 1047–52, 1054. PMID 10706157. Archived from the original on 13 April 2014. Retrieved 24 August 2012.
- ↑ 4.00 4.01 4.02 4.03 4.04 4.05 4.06 4.07 4.08 4.09 4.10 4.11 4.12 4.13 Brook, I. (2002). "Microbiology and management of acute suppurative thyroiditis in children." International Journal of Pediatric Otorhinolaryngology, 67, 447-451.
- ↑ 5.0 5.1 5.2 5.3 5.4 5.5 5.6 5.7 Pearce, Elizabeth M.D., Alan P. Farwell M.D. and Lewis E. Braverman M.D. "Thyroiditis." The New England Journal of Medicine. 2003 June 26;348:2646-2655.
- ↑ 6.0 6.1 6.2 6.3 Park, Sun W., Moon H. Han, Myung H. Sung, In O. Kim, Kwang H. Kim, Kee H. Chang, and Man C. Han. "Neck Infection Associated with Pyriform Sinus Fistula: Imaging Findings." American Journal of Neuroradiology Am J Neuroradiol 21 (2000): 817-22.
- ↑ 3) Lazarus, John, and James Hennessey. "Acute and Subacute, and Reidel’s Thyroiditis." Ed. Leslie J. De Groot. The Thyroid And Its Diseases. 6th ed. New York: Elsevier, 1996
- ↑ Yamada, H., Fujita, K., Tokuriki, T., & Ishida, R. (2002). "Nine cases of piriform sinus fistula with acute suppurative thyroiditis." Elsevier, 29, 361-365.
External links
| Classification |
|---|
- Pages with script errors
- All articles with dead external links
- Articles with dead external links from October 2016
- Articles with invalid date parameter in template
- Articles with permanently dead external links
- All articles with unsourced statements
- Articles with unsourced statements from August 2020
- Thyroid disease